Resistant hypertension (RH) presents a critical challenge in modern cardiovascular care, affecting approximately 5% of individuals with high blood pressure.
According to the NIH, RH is defined as systolic blood pressure (SBP) remaining above 140 mmHg or diastolic blood pressure (DBP) above 90 mmHg. This occurs despite adherence to lifestyle changes and treatment with optimal or maximally tolerated doses of three antihypertensive medications, including a diuretic.
RH is not only difficult to control but is also linked to significantly higher risks of cardiovascular complications. Driving better results in RH treatment is essential to reducing morbidity and improving patient outcomes.
Understanding the Complexity of Resistant Hypertension
Resistant hypertension is a multifaceted condition that complicates standard hypertension management. Its complexity stems from various overlapping causes and population-level disparities.
According to Frontiers, this condition affects an estimated 100–500 million people globally. It places immense strain on healthcare systems due to its complications and the increased risk of morbidity and mortality.
Key aspects of RH include:
- Underlying contributors: Non-adherence to medication, inappropriate drug combinations, and secondary causes like sleep apnea, primary aldosteronism, and renal artery stenosis.
- Pseudo-resistance: Blood pressure may appear uncontrolled due to errors in measurement or medication timing.
- Associated conditions: Chronic kidney disease, thyroid disorders, obesity, excessive sodium intake, and alcohol use.
- Demographic disparities: More common in older adults, men, and people with diabetes, kidney disease, or from African American and Hispanic communities.
- Pathophysiology: Involves sympathetic nervous system overactivity, volume overload, and arterial stiffness.
Advanced Diagnostic Approaches
Accurate diagnosis is critical in managing resistant hypertension, as misclassification can lead to inappropriate treatment strategies. Modern diagnostic techniques focus on validating elevated blood pressure and uncovering contributing factors. According to the BMJ, the evaluation process should include:
- Proper blood pressure measurement: Errors such as incorrect cuff size or arm positioning can falsely elevate readings.
- Exclusion of white coat effect: Ambulatory blood pressure monitoring (ABPM) or properly conducted home blood pressure monitoring is essential to confirm true hypertension.
- Automated office blood pressure (AOBP): This method uses oscillometric devices to take multiple readings in a quiet, unattended setting. AOBP closely aligns with home measurements and minimizes white coat influence.
- Assessment of medication adherence: Diagnosing true resistant hypertension requires confirmation that patients are consistently taking prescribed medications.
By employing these evidence-based diagnostic tools, clinicians can distinguish between pseudo-resistance and true resistant hypertension, enabling more targeted and effective interventions.
Innovative Treatment Strategies
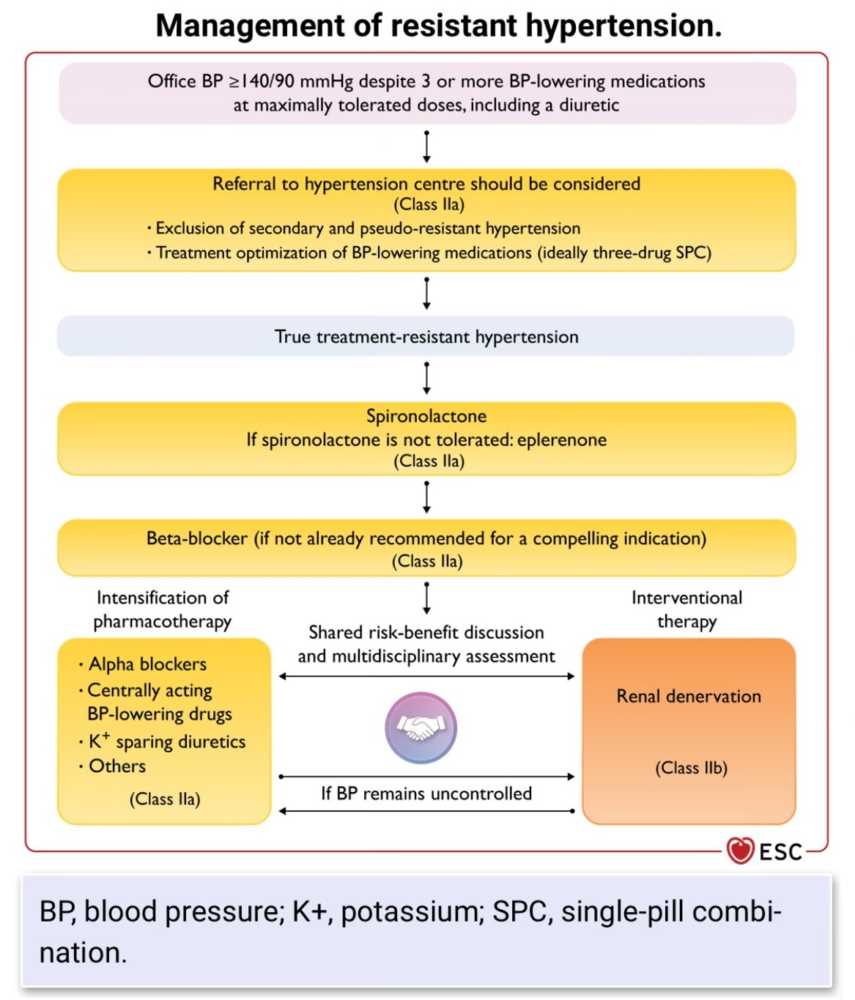
The treatment landscape for resistant hypertension (RH) is rapidly expanding with novel therapeutic approaches. When medication optimization falls short, device-based therapies offer a promising alternative. They include:
- Renal denervation: A minimally invasive procedure using radiofrequency or ultrasound energy to disrupt renal sympathetic nerves, helping lower blood pressure by reducing sympathetic overactivity. It’s shown promising results when paired with optimized medical therapy.
- Baroreflex activation therapy: This implantable device stimulates carotid baroreceptors to regulate blood pressure naturally. It is adjustable and reversible, offering personalized control in resistant cases.
Pharmacological innovations also play a crucial role. Fixed-dose combinations enhance adherence by reducing pill burden, while extended-release formulations offer consistent 24-hour control. Additionally, mineralocorticoid receptor antagonists like spironolactone and eplerenone have become prominent fourth-line agents in the management of resistant hypertension.
They effectively address volume overload and aldosterone excess, which are common contributors to treatment resistance.
Adding to these strategies, Medscape highlights the QUADRO study, which demonstrated the effectiveness of a four-drug full-dose combination in a single pill. This regimen, perindopril, indapamide, amlodipine, and bisoprolol, was shown to lower blood pressure more effectively than the standard triple combination. These diverse innovations are vital for achieving better results in complex RH cases.
Multidisciplinary Collaboration for Complex Cases
The growing complexity of resistant hypertension has highlighted the need for an integrated, team-based model of care. This condition often involves multiple comorbidities and treatment challenges that cannot be adequately addressed by a single provider.
Effective management demands the combined expertise of various healthcare professionals who can assess different aspects of the patient’s condition and coordinate interventions. Within this framework, nurses play a pivotal role in improving outcomes through direct patient engagement, education, and clinical monitoring.
Specialized hypertension nurses act as case managers, facilitating communication across disciplines while guiding patients through every step of their treatment.
Their responsibilities include medication reconciliation, identifying drug interactions, monitoring side effects, and teaching patients accurate home blood pressure monitoring. For nurses aspiring to take on leadership roles in managing chronic conditions like resistant hypertension, MSN-FNP programs provide specialized training.
According to Spring Arbor University, these programs prepare nurses to deliver population-specific care and promote health equity. They also empower nurses to guide patients through behavioral change using a compassionate, family-focused approach.
Lifestyle Modifications and Patient Engagement
Managing resistant hypertension effectively goes beyond medication, requiring sustained lifestyle changes and active patient engagement.
According to the American Heart Association, patients should:
- Eat a well-balanced diet
- Limit alcohol
- Enjoy regular physical activity
- Manage stress
- Reach and maintain a healthy weight
- Quit smoking (or avoid starting)
- Take medications properly
- Collaborate with healthcare professionals
Digital tools like apps and telehealth help sustain these changes through real-time support.
Frequently Asked Questions
What are the outcomes of resistant hypertension?
Resistant hypertension significantly increases the risk of adverse health outcomes, including stroke, heart failure, chronic kidney disease, and cardiovascular events.
Poorly controlled blood pressure despite treatment can lead to target organ damage and reduced quality of life. It also contributes to higher mortality rates, underscoring the need for aggressive and comprehensive management.
Does resistant hypertension go away?
Resistant hypertension may improve with comprehensive management, including medication optimization, lifestyle changes, and addressing secondary causes. While it rarely “goes away” entirely, many patients can achieve better blood pressure control through multidisciplinary care, consistent monitoring, and treatment adherence. Long-term success depends on individual factors and ongoing medical support.
Which types of exercise are effective for managing high blood pressure?
Consistent physical activity plays a vital role in controlling high blood pressure. Aerobic exercises like brisk walking, swimming, cycling, and dancing effectively lower blood pressure. Strength training with weights or resistance bands boosts heart health. Flexibility exercises like yoga and stretching enhance overall fitness, reduce stress, and support cardiovascular well-being.
The treatment of resistant hypertension requires a comprehensive, multifaceted approach that combines advanced diagnostic techniques, innovative interventions, and coordinated multidisciplinary care. Success depends on accurate identification of contributing factors, optimization of medical therapy, appropriate use of device-based interventions, and intensive lifestyle modifications.
The critical role of nurses and other healthcare team members in providing education, monitoring, and care coordination cannot be overstated.
This article is a guest contribution submitted by a professional healthcare writer and reviewed for accuracy.

![Read more about the article Left Ventricular Hypertrophy (LVH): How to Recognize it on ECG [With Examples]](https://manualofmedicine.com/wp-content/uploads/2025/12/Summary-of-the-various-diagnostic-ECG-criteria-for-left-ventricular-hypertrophy-LVH.png)