This is an Answer to the Case – Black Pleural Effusion .
A 56-year-old man undergoing treatment for a prostatic acinar adenocarcinoma was referred for assessment of a massive right pleural effusion. Although the effusion was large, he had only mild shortness of breath and was admitted originally for urinary incontinence.
A pleural aspiration showed black pleural fluid. This fluid was determined to be an exudate with very high concentrations of protein (85 g/L; serum protein 56 g/L), lactate dehydrogenase, and amylase. The doctors drained about 3 L of this black pleural fluid from the patient over the following 24 h.
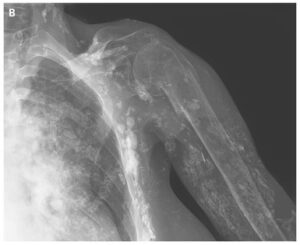
Fibreoptic bronchoscopy was normal. However, a thoracoscopy showed nodularity of the visceral and parietal pleura with significant pleural thickening.
Pleural fluid cytology showed groups of neoplastic cells arranged in balls, gland, and papillioid configuration in a haemorrhagic background with mesothelial cells and mixed population of inflammatory cells.
Immunohistochemistry studies favoured a diagnosis of an adenocarcinoma of pulmonary origin. Percutaneous and thoracoscopic pleural biopsies also confirmed this diagnosis.
Black pleural effusions are extremely rare and have been reported previously in patients with:
- Pleural infections caused by Aspergillus niger and Rhizopus oryzae,
- Metastatic melanoma
- Adenocarcinoma of the lung
- Pancreaticopleural fistula
- Oesophageal perforation during activated charcoal treatment for a drug overdose
- Patients actively using crack cocaine
The black pleural fluid in our patient was most likely due to haemolysis and the presence of haemosiderin-laden macrophages after a massive bleed into the pleura.
The absence of clinically significant symptoms in spite of the massive effusion and the fact that the fluid was black and not red suggest that the fluid collected over a prolonged period of time and that the bleeding would have occurred a long time before presentation.
Increased concentrations of amylase in the pleural fluid, as noted in our patient, are commonly seen in patients with lung cancer—most frequently in those with adenocarcinomas.