On repeated examination, it was noted that the patient had swelling of the left upper eyelid, conjunctival congestion, restricted abduction of the left eye, which is diagnostic of a left sixth cranial nerve palsy, and binocular horizontal diplopia.
The rash was distributed over the left frontal area. The rest of the eye examination, including extraocular movements, visual acuity, visual field, pupillary evaluation, and funduscopy, was normal.
The blood glucose level, erythrocyte sedimentation rate, and C-reactive protein level were normal.
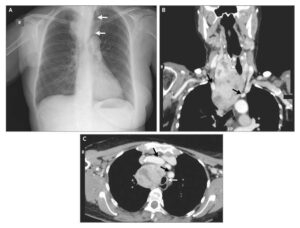
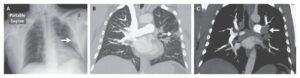
A computed tomographic scan of the paranasal sinuses and orbits showed thickened mucosa of the sinuses but was otherwise unremarkable. A diagnosis of herpes zoster ophthalmicus was made.
The patient was treated with gabapentin and acyclovir for one week. Six weeks later, he had minimal residual diplopia, with no postherpetic neuralgia.
It is important that this diagnosis be made early, to minimize complications such as corneal ulceration and uveitis, which may threaten vision.